Electronic General GP Referrals - Cork & Kerry Pilot
Introduction
The Hayes Report in March 2010 into “unopened” or “unprocessed” GP referrals in Tallaght Hospital, and the subsequent HIQA report on patient referral from GPs to outpatient services highlighted a number of problems which needed to be addressed, including:
- Failures in communication
- Lack of visibility and traceability of referrals
- Significant variation and lack of protocols for the management of referrals between sites
This case study outlines how the National Electronic General GP Referral Pilot Project tackled these problems using technology to bring about significant patient centered benefits to seven acute hospitals in Cork, Kerry and Tallaght, and participating GPs and addressed recommendations in these reports.
The Challenge
Initial scoping of the referral pathway by the project team included:
- workshops attended by over 170 staff and patients involved in referral management in GP practices and hospitals
- a survey of all Cork, Kerry and Tallaght area GPs
- site visits to observe areas of good practice for the processing of GP manual referrals
- step by step process mapping of how different specialties and different hospitals managed referrals
The team found:
- massive variation in processes
- a lack of visibility and traceability of where referrals were during the process
- lack of clarity regarding who was responsible for the patient during this time
- unnecessary communication between GPs, patients and hospitals as updates were not provided to the GP or patient along the way
- GPs reported sending duplicate referrals for the same patient as they were unsure of the outcome of each referral
“a referral might go through 11 handovers before a patient received an appointment”
The Solution
The National Electronic General GP Referral Project Team and National Advisory Group (see below) included stakeholders from each facet of the care pathway and those who were involved in developing previous electronic referral systems. They were tasked with assessing the current outpatient’s referral pathway and developing a standardised end-to-end process which would safely enable the introduction of electronic general referral.
In order to decrease the variability inherent within the existing processes the project team focused on the following elements:
- Using the general referral form developed by HIQA in association with ICGP
- Integration of this form into four accredited GP Practice Management Systems (Socrates, Helix, HealthOne and Complete GP).
- Development of a Healthlink on-line electronic general referral form.
- The introduction of mandatory fields in the referral to strengthen the quality of information received by hospitals.
- Delivery of electronic general GP referrals to hospitals using Healthlink, the national messaging system.
- Development of a standard end-to-end process within hospitals to manage electronic referrals in a consistent, traceable, timely and efficient manner with a clear governance structure put in place.
- Development of associated feedback mechanisms and performance metrics to monitor the system.
Ensuring project buy-in by stakeholders was a priority of the project as significant process change was required from the hospitals and GPs alike. A communications and engagement strategy was developed to ensure that GPs, patients, hospital staff, unions and others were involved in developing the solution collaboratively
 |
OPD Supervisor in the Mercy Hospital Cork with a GP eReferral letter |
Process Improvements
Six Sigma Lean Management principles were used to refine multiple processes with varying degrees of complexity into one standard solution through continuous improvement methodologies and the continued gathering of feedback from service users which was acted upon wherever possible. Abtran, a local industry partner, were involved in the development of the pre test process. The Mercy University Hospital was the first site to go live. As a soft launch pilot site learning was gathered and the system improved prior to roll out to other sites.
Historic manual OPD referral processes:
- contained between 10 and 20 process steps (depending on the specialty)
- Had up to 11 touch points (people handling each referral)
- took up to 28 working days to complete registration and triage
- cost €13.22 in total per referral
The re-engineered electronic referral process:
- now contains between 8 and 12 process steps
- now has between 4 and 6 touch points,
- the duration for the majority of referrals is now between 4- 6 working days to complete registration and triage
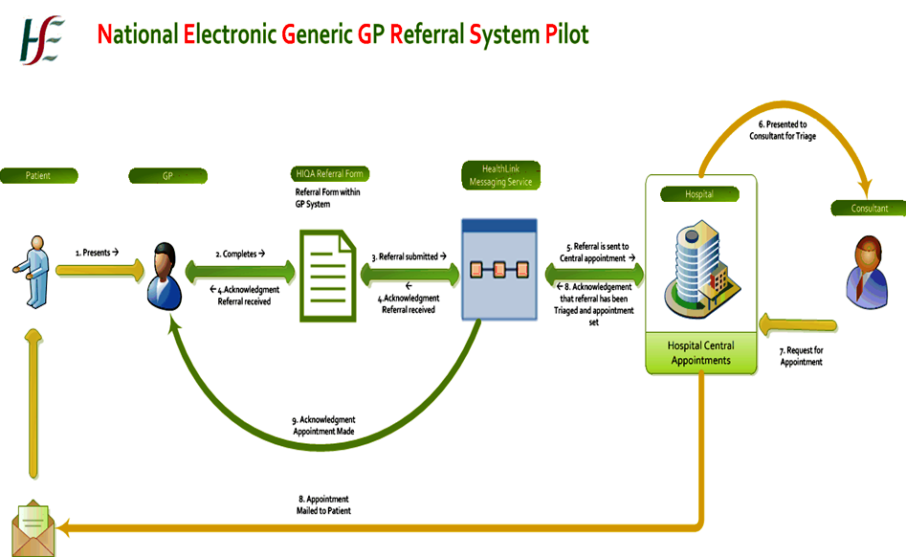
Benefits For All
Patients
GPs
Hospitals:
|
 |
Conclusion
The project was a huge success and clearly demonstrates some of the key deliverables of the eHealth Ireland Knowledge and Information strategy:
- Care Delivery Enablement - It provides a clinical and care delivery capability which generates electronic referrals previously manual processes thereby allowing electronic data capture, better quality of care, more clinician time spent with the patient and a greater ability for patients to participate in their own care.
- Cross Setting Information Integration - Delivers the required integration, information flows and process standardisation across care settings, enabling the summary care record at a patient level, and seamless patient transition between settings.
- Health Service Intelligence- Delivers the information management, reporting and analysis solutions and processes which provide timely, reliable information and decision support for patients, clinicians, and management from the micro level (e.g. individual patients or treatments) up to the macro view (e.g. system wide performance, population health trends, demand and capacity planning).
Next Steps
The newly appointed CIO of the HSE, Mr. Richard Corbridge, visited Cork in January 2015 and strongly endorsed the pilot solution. He commended the project team on their achievements to date, noting the lack of full time staff dedicated to the project, and comparing it to the 100+ NHS staff who worked on “Choose & Book”, an electronic referral project in the UK, for over a year. He proposed the national roll out of the pilot solution on a phased basis and has appointed a project manager, Gregory Johnston, to complete this within 12 months. The next 6 sites are now live with plans to take all acute hospitals live by March 2016.
Acknowledgements
*Following an open tender process, Abtran, a company specializing in business process re-engineering, worked closely with the project team in the first 18 months of the project to assist with mapping the original process and developing the standardized solution to enable successful introduction of electronic general referral

Contacts
| Elaine Naughton, Office of the CIO | @NaughtonElaine | elaine.naughton@hse.ie |
| Dr. Joe Clarke, Clinical Co-Chair | joe.clarke@hse.ie | |
| Sinead Glennon, Management Co-Chair | @sineadg163 | sinead.glennon@hse.ie |
| Joyce Healy, Project Manager | @oriordainjoyce78 | joyce.healy@hse.ie |
| Gregory Johnston, Project Manager National eReferral Project | ereferrals@ehealthireland.ie |
- Ambulance Arrivals Project A Case Study
- SNOMED National Release Centre (NRC)
- SVUH Award winning Patient Flow Whiteboard
- Scan for Surgery
- Hospital-based care
- Digital Natives Sign App
- Digitisation of risk assesment tools for Adult mental health services in north Dublin
- Patient Engagement Operating Systems - Hep C
- Digital Transition for HSCPs at St. James's Hospital
- Primary Care Centre Castlebar Case Study
- Mario - Managing active and healthy ageing using caring service robots
- Claimsure - Health Insurance Claims Management System
- Cyber Attack Response
- Data systems in SVUH Emergency Department
- Electronic Discharge Prescription Pilot
- Epilepsy EPR
- eReferral
- eReferral Radiology Pilot
- eRostering
- Electronic Blood Tracking
- GP Practice Management Systems
- Healthmail
- Heart Failure Virtual Clinic
- Infrastructure - MPUP to ECAM
- IT Security - Small changes, big difference
- Kidney Disease Clinical Patient Management System
- Local Asset Mapping Project at St James' Hospital
- LUCY
- Mi Kidney App
- Model Community
- NCHD - Employment Record Portal
- Nursing & Midwifery Quality Care Metrics
- Ophthalmology Electronic Patient Record
- PharmaBuddy
- Radiology & Electronic Patient Record
- National Smart-Pump Drug Library of Paediatric and Neonatal Standardised Concentration Infusions
- Quality & Patient Safety
- Robotic Assisted Surgery Programme
- Shared Learning on EHR
- St. James' Hospital - National Haemophilia System
- Tallaght Hospital Pharmacy
- Tallaght Hospital Patient Engagement App
- Track & Trace
- Using IT to Improve Ireland's Public Sector Healthcare
- National Audiology Clinical Management System (NA-CMS)
- St Vincent's University Hospital Award Winning Whiteboard Patient Flow System
- Snomed Case Study
- Telehealth Project Donegal
- St Vincent's Whiteboard Patient Journey System a Case Study
- Ambulance Arrivals Project


